-
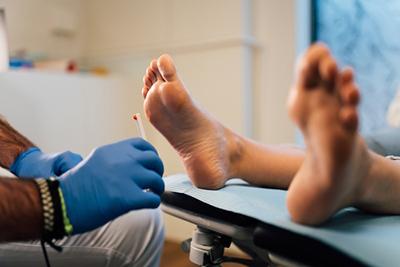
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 08, 2024.

-
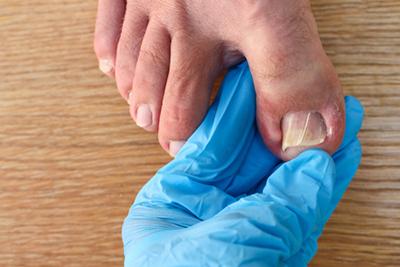
Ingrown Toenails: Prevention Tips and Treatment Options
posted: Apr. 03, 2024.
-
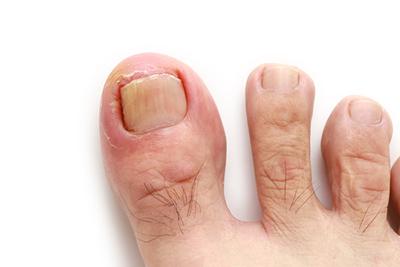
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
-
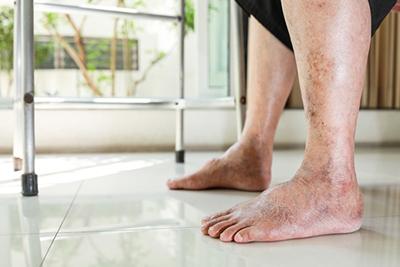
Treating Foot Arthritis: Management Strategies for Pain Relief and Mobility
posted: Mar. 23, 2024.

-
Diabetic Foot Care: Managing Risk Factors and Preventing Complications
posted: Mar. 21, 2024.
-
Treating Plantar Fasciitis
posted: Mar. 15, 2024.
-
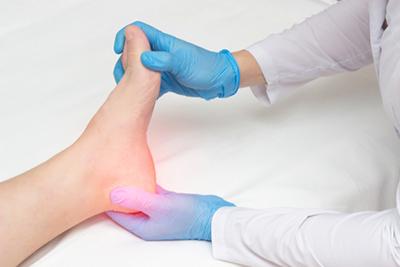
Managing Your Heel Pain
posted: Mar. 01, 2024.
-
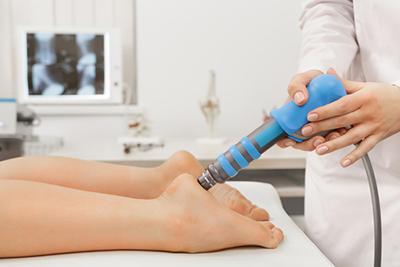
The Role of Podiatry in Managing Foot and Ankle Fractures
posted: Feb. 12, 2024.
-
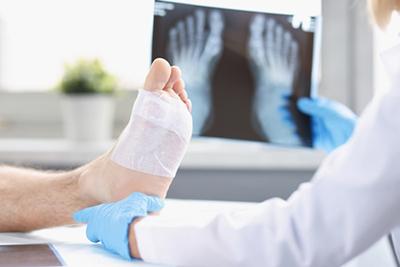
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
-
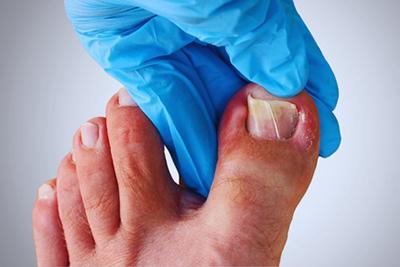
When To Seek Professional Help for Foot Pain
posted: Jan. 14, 2024.
-
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
posted: Jan. 12, 2024.

-
Understanding Bunions: Causes and Risk Factors
posted: Jan. 10, 2024.
-
The Importance of Regular Podiatric Check-ups
posted: Jan. 08, 2024.

-
A Guide to Preventing Ingrown Toenails
posted: Jan. 05, 2024.
-
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.

-
Dealing With Plantar Fasciitis
posted: Dec. 23, 2023.

Contact Us
Send us an email today!
OUR LOCATIONS
Find us on the map
HOURS OF OPERATION
Our Regular Schedule
Hampton Roads Foot and Ankle Specialists
Monday:
8:30 am-4:30 pm
Tuesday:
8:30 am-4:30 pm
Wednesday:
8:30 am-4:30 pm
Thursday:
8:30 am-4:30 pm
Friday:
8:30 am-12:00 pm
Saturday:
Closed
Sunday:
Closed
